It’s no secret in the healthcare industry that provider reimbursements have been shrinking.¹ At the same time, health care costs are expected to rise 6.5% through 2017, outpacing the rate of inflation.²
In light of this, many analysts believe it was inevitable that health systems would start moving toward integrated network models, with their focus on reduced costs and optimized patient care.³
Here are 3 trends to watch for in integrated networks in the next few years.
1. A Growing Number Of Value-Based Care Contracts
The fee-for-service model continues to dominate the landscape, but that model is slowly changing.4
By the end of 2016, 30% of fee-for-service Medicare payments will move to a value-based payment model.5
These contracts essentially give providers an incentive to reduce expensive or unnecessary procedures and promote preventative care.
Private insurance plans are making a similar shift:6
- In 2013, 11% of payments in commercial insurance plans were value-oriented.
- By 2020, a new coalition of private insurers, including Aetna and Blue Cross, aims to transition 75% of their contracts into alternative reimbursement models.
For providers in clinically integrated networks like Children’s Health Network, the good news is that these organizations are positioned to protect physicians in this cost-conscious environment through:
- Quality improvement projects led by physicians
- Care standards driven by sophisticated population data
- Clinical efficiency studies
- Preventative care outreach programs
2. Improving Analytics
When a network’s reimbursements depend on data and outcomes, analytics are becoming even more critical.7 Watch for more business intelligence, predictive analytics, and population health management.
Also expect to see more healthcare wearables and interactive tools, such as FitBit or weight scales, that transmit data to physicians. This “Internet of Things” market segment is expected to reach $177 billion by 2020.8
At the same time, Electronic Medical Records (EMRs) are becoming “smarter.” Beyond simply displaying patient raw data, they’re running quantitative models that flag physicians on risk and other information relevant to the patient’s care.9
Read more about Children’s Health Network’s Healthy Planet data warehouse.
3. New Avenues For Engaging Patients
Correct analytics depend upon the health system’s ability to see the patient at every touchpoint of care, from routine physicals to complex surgery.
When patients go outside the health system, this can complicate the network’s ability to track data, adjust care standards, and manage costs.10
As time goes on, watch for clinically integrated networks to forge creative new paths to their patient populations, such as virtual care.11
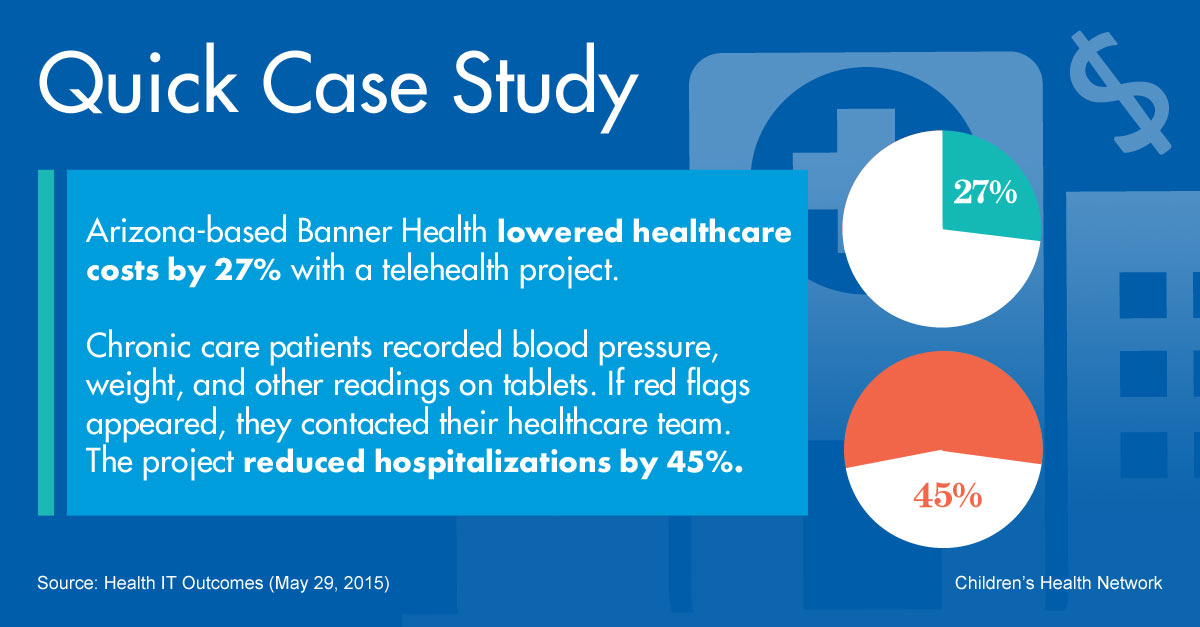
All About Connections
Healthcare Financial Management Association mentions outside-the-box smartphone technology that lets diabetic patients upload their blood sugar readings to their electronic health records and get feedback from a healthcare coach.12
Then, there’s old-fashioned face-to-face outreach.
Partners for Kids, an accountable care organization based in Ohio, offers a program that lets children receive their asthma medication at school.13 It also trains parents in how to dispense the medication at home.
The organization says this effort has raised school attendance rates and reduced emergency room visits. And it has provided valuable population data for the health system.
Expect to see more innovative patient outreach as the payer-reimbursement focus keeps shifting to wellness. Physicians say developing programs like these is a chance to make a strong impact on health policy and patient care for many years to come.
1 Hospitals & Health Networks (Jan. 13, 2015)
2 Fortune (June 21, 2016)
3 Medical Economics (Feb. 10, 2016)
4 Becker’s Hospital Review (March 7, 2016)
5, 6 Committee for Economic Development (August 2016)
7, 8 Healthcare IT Leaders (Jan. 11, 2016)
9 HealthData Management (Dec. 21, 2015)
10 Healthcare Financial Management Association (2016)
11, 12 HFMA (June 29, 2016)
13 Nationwide Children’s (August 2016)