COVID-19 Update for Providers: All patients who have had COVID-19 should consult a provider before returning to play. Learn more about return to play.
Some adolescents play sports. Some adolescents live them. We get that! The last couple of decades have seen an increase in athletic participation among adolescents and teens. That also means an increase in youth sports-related injuries. The Sports Medicine Program at Children’s Nebraska is the best place for young athletes with sports-related injuries, such as concussions, sprains, and overuse injuries. Our pediatric sports medicine specialists are here to provide a complete and accurate diagnosis, with a plan to get your young athlete back to play as quickly and safely as possible.
Make An Appointment
Clinic Hours
Omaha: 8 a.m. – 4:30 p.m.
Phone 402-955-PLAY (7529) | Fax 402-955-6529
Our Specialists

About 2 million injuries occur among high school athletes each year.
More than 3.5 million US children under age 14 get hurt every year while playing sports.
About half of these sports injuries can be prevented. Ask us how.
What Sets Children’s Apart?
Our Pediatric Sports Medicine team is made up of experts who specialize in age-appropriate treatment and prevention of injuries to young athletes. We understand the nature of sports and share our patient’s determination to return them to the field of play.
We know young athletes:
- Are still growing: Proper diagnosis and treatment of growth plate injuries is crucial to preventing long-term side effects
- Experience different injuries or conditions specific to periods of rapid growth
- Are predisposed to certain types of fractures that differ from those of older athletes
When your young athlete comes to the Children’s Sports Medicine Program, they will be treated by an entire team of pediatric sports medicine specialists, including specially trained sports medicine physicians, orthopedic surgeons, and athletic trainers. They will also have access to pediatric sports medicine nurses.
We also offer Sports Physical Therapy, the only program of its kind in the area dedicated solely to treating pediatric and adolescent sports injuries.
Conditions We Treat
We see many different types of injuries in sports, from sprained ankles to traumatic brain injuries. The conditions we see include:
-
Concussions
Concussions are traumatic brain injuries that occur when a blow or jolt to the head or body causes the brain to bounce off the skull. These are serious injuries that can affect how the brain functions.Many concussions heal on their own by modifying activity, as long as the head does not get hit again while healing. However, depending on the extent of the damage to your adolescent’s brain, they may need physical, speech, or occupational therapy.
Learn more about concussions,including our concussion clinic at Children’s Hospital.
-
Heat Illnesses
Heat illnesses occur when your adolescent is exposed to extremely high temperatures and humidity, and their body is unable to cool down. Heat illnesses can range in severity, from mild cramps to life-threatening heat stroke.Learn more about heat illnesses.
-
Musculoskeletal Injuries
Any injury that occurs to a skeletal muscle, tendon, ligament, bone, joint, or nerve is a musculoskeletal injury. Sprains, strains, and overuse injuries in sports are some of the most common types of musculoskeletal injuries.- A sprain is the stretching or tearing of a ligament (the band of tissue that connects two bones together). Sprains are found in and around the joints (e.g., ankles, knees, wrists).
- A strain is the stretching or tearing of a muscle or tendon (the cord of tissue that connects bones to muscles). Strains are common in the back or hamstring muscles.
- An overuse injury is damage to a bone, muscle, tendon, or ligament that is caused by repetitive stress without allowing the body time to heal. Your adolescent may get an overuse injury if they play a sport where their position requires constantly using the same body part (e.g., a pitcher in baseball). Types of overuse injuries in sports include shin splints, tendonitis, and stress fractures.
Wondering about the four stages of an overuse injury or what can cause overuse injuries in children? Learn more about musculoskeletal injuries, which includes overuse injuries.
-
Sports-Related Infections
These are infections that your adolescent gets while playing a sport. There are a number of reasons why an athlete may develop an infection, including skin-to-skin contact, sharing equipment and towels, or poor hygiene. Symptoms depend on the type of infection and may involve blisters, sores, warts, or red, itchy skin.Learn more about sports-related infections.
-
Sudden Cardiac Arrest
Sudden cardiac arrest occurs when your adolescent’s heart suddenly develops a dangerously high heart rate, causing the heart to stop effectively pumping blood throughout the body. It usually happens because of an undiagnosed heart disorder. Since sudden cardiac arrest is more likely during exercise or physical activity, athletes are at an increased risk.Learn more about SCA and other cardiac issues.
Treatments And Services
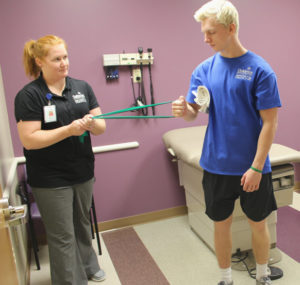

Our Sports Medicine Program providers will work with your young athlete to create a game plan that covers all aspects of treatment.
The Sports Medicine Program offers:
- X-ray capability to view and diagnose injuries, which we can perform on-site, meaning you won’t have to make a separate trip to the radiology department
- Immediate surgical assessment with orthopedic and sports medicine surgery specialists
- Crutch fitting and gait (walking and moving) training to help decrease stress on lower-body injuries, and increase the speed of healing
- On-site application of any brace, cast, or splint needed for support or protection during recovery or play
- Home exercise programs taught by licensed athletic trainers to help your young athlete get a jumpstart on the recovery process, increase the speed of healing, and return to play safely
- Diagnostic and therapeutic ultrasound for appropriate conditions
- Sports physical therapy (Children’s physical therapy is the only program in the area solely dedicated to sports injuries in children and teens.)
Community Resources
Partnerships
We work with coaches, parents, athletic trainers, and school administrators to provide treatment for concussions and sports injuries. We also provide programming to prevent injuries from happening in the first place.
When schools, teams, and athletic organizations partner with our Sports Medicine Program, they receive:
- Access to care from our team members, who are leaders in sports medicine
- Educational programming for issues facing student athletes today, including:
- Sports nutrition
- Hydration
- Concussion education
- When is an injury really an injury
- Injury prevention training
- Resources for sport-specific training and conditioning
- Electronic resources with the latest information on issues facing young athletes today
- Priority appointment scheduling
Are you interested in becoming one of our partners? For more information, please contact our Sports Medicine Coordinator, Kerry Waple, MEd, ATC, CSCS, at 402-955-6574 or [email protected].
Speakers Bureau
True to our mission of being a global leader in healthcare for children and adolescents, the sports medicine experts at Children’s are available for educational presentations to your team or group. We have the most up-to-date information to share on topics ranging from concussions, to nutrition and diabetes, to distance running. As advocates for young athletes, we are here to help enhance their athletic experience and keep them safe.
Here are a few examples of the topics we have available to provide educational sessions on:
- Sports injury prevention
- Strength training for young athletes
- Sports nutrition
- Hydration tips for extended play
- Concussion identification and management
- Emergency action planning
- Sports specific injuries
- Dynamic warm-ups and stretching for sports
- Prevention of shoulder injuries in the throwing athlete
- Overuse injuries in youth sports
- Supplement use in sports
- Sports injury care
Please let us know if you have a particular need, and we can customize a session for you.
Sports Medicine Library
- Blister Care
- Cast and Splint Care
- Coach’s Guide to Sports Injuries
- Crutch Safety Tips
- Dental Injuries and The Role of Mouthguards
- Female Athlete Triad
- Game Day Fueling Plan for Athletes
- Fit Fore the Fairway
- Healthy Snack Choices for Youth Sports
- How to Choose a Running Shoe
- Hydration for Sport
- Little League Elbow
- Little League Shoulder
- Making Healthy Food Choices on the Road
- Overuse Injuries
- The Diabetic Athlete
- The Game Plan
- Throwing Guidelines for Young Players
- Tips for New Runners
What To Do Next
For Patients
When To Make An Appointment
There are several signs that indicate that your young athlete should be seen by one of our pediatric sports medicine specialists:
- They exhibit signs of a concussion (e.g., seizures, vomiting, headache that gets worse, confusion, difficulty waking up, loss of consciousness).
- Pain or swelling from an injury does not improve, or increases in intensity, despite standard treatment measures — rest, ice, compression, elevation, (RICE) and decreased activity.
- Pain persists longer than 10 to 14 days.
- Pain resolves with rest but flares back up when activity resumes.
- They must take pain medication to train or compete without pain.
To get your young athlete back in the lineup as quickly and safely as possible, we are often able to schedule same-day appointments. We also do not require a referral from your adolescent’s physician.
Call 402-955-PLAY (7529) to schedule an appointment.
What To Bring To The First Appointment
Please bring the following items to your adolescent’s appointment:
- Insurance card
- Medical records or imaging from other providers who have seen your adolescent for this injury
For Providers: Return to Play After COVID-19
All patients who have had COVID-19 — whether recently or at the beginning of the pandemic, and whether it was severe or asymptomatic — should consult a provider before returning to play. Take this assessment to see if your patient should see a primary care provider, sports medicine provider, or cardiologist.
Other Information
Your Young Athlete Recovered From COVID-19 And Is Ready To Return To Play. Now What?
For Referring Providers
The Physicians’ Priority Line is your 24-hour link to pediatric specialists at Children’s for emergency and urgent consults, physician-to-physician consults, admissions, and transport services. Call 855-850-KIDS (5437).
Learn more about referring patients.

